|
Hypoglycemia - This condition occurs when a neonate has low levels of blood sugar. Glucose blood levels can drop in neonates for the following reason:
All information retrieved from the NIH
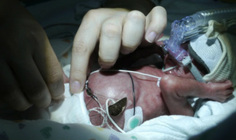
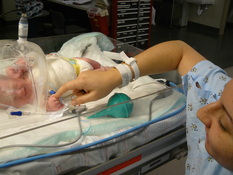
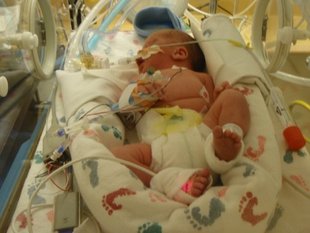
 On May 6, 2012 our son Kaleb was born at 24 weeks weighing just 1 lb 12oz. After he was born he was transported to the NICU where he spent the next 110 days. We knew that it was going to be a long bumpy road and we weren’t too sure what issues to expect, but I can tell you that MRSA was not one of them! For those who may not know MRSA is a bacteria that can cause infections in different parts of the body and although most cases are not serious some can be life threatening and it is very difficult to treat. Everyday my husband Mike and I went to visit Kaleb and it had become a routine, from the parking to the elevator ride, then washing our hands for 3 minutes, and then right into see Kaleb, first bed on the right. This time we went in and he was not there which of course sent us into a panic. The nurses informed us that he had been moved into isolation because he tested positive for MRSA. We have no idea how he got MRSA, all we knew was that Kaleb and another baby were placed into isolation for testing positive. The nurses told us that sometimes it does happen and it could have been a number of things that attributed. At the time they had let us know that he was only colonizing it and that it was not making him as sick as it could at the moment, but he needed to be in isolation so that that other babies were protected. What this meant for us was that when we visited him we had special gowns we needed to wear, we had to wear gloves, and there was extra washing of our hands every time we left the isolation room. This was very difficult for us because putting our hands in Kaleb’s isolette was the only way we were able to connect with him and it was hard to feel him through the gloves we needed to wear. At this time, Kaleb was already 3 weeks old and we had yet to be able to hold him and MRSA prolonged that as well. A few times a day the nurses would swab all the key areas where the MRSA grows with medication and hope that the tests would finally come back negative. He was tested every week and in order to get out of isolation and be in the clear Kaleb needed to have 2 weeks worth of negative test results in a row. After 3 weeks in isolation he finally had a negative result and although we still needed to wait for a second week worth of negative test results, the current results meant that we were finally allowed to hold him! We had been waiting for this day for weeks and it was such a happy yet emotional moment! Because he was still in isolation we still needed to wear the special gown and the gloves, but being able to finally hold our baby for the first time was still an amazing feeling! The following week, Kaleb’s test results came back negative and he was finally, after 4 weeks, able to leave isolation. We were told that because he was colonizing it now, he would always colonize it and that would be something that we would need to keep an eye on throughout his stay in the NICU as well as the rest of his life. After his issue with MRSA, Kaleb spent another 2 ½ months in the NICU without any further issues or positive test results for MRSA! Today, Kaleb is your typical 2 year old little boy with scraped knees and a dirty face, running and playing just like any other child his age would be and although he went through many difficulties throughout his life thus far, we are just happy that he is happy and healthy!
Information Retrieved from NIH
 How do you inform your children that their new sibling may not be coming home from the hospital as quickly as you had thought? Take a bit of time to react to the diagnosis, and arm yourself with information and support to help share the news. Children are very intuitive, and also very resilient. Be as open and honest as you can possibly be, in simple, age appropriate language that they can understand. Preparing how you explain it to your child(ren) is important. Choose your wording carefully to avoid confusion as children often take things very literally. Avoid making promises that you do not know you can provide to avoid future frustration and confusion. Allow them to express their feelings openly and let them know that you are always available to answer their questions, and provide the necessary comfort they may be seeking. Make time for the siblings, as they often become or feel like the "forgotten ones" while their new baby is in the hospital. It’s important that in the chaos they still have some individual attention. Reach out to family and friends and request their assistance with the child-rearing responsibilities as well. There will be times when your emotions may spill out in the presence of your children. This is normal and unavoidable at times. Be gentle with yourself as you comfort and reassure them that you're there for their needs, and that expressing emotions is "okay". It’s common for siblings to act out and have behavior issues during this time. Having a NICU baby affects the whole family. Seek outside assistance, if in doubt, through your local health provider or children's mental health services. Professionals will be able to recognize anything which may be concerning, and recommend/provide necessary supports and helpful resources.  Breastfeeding In The NICU Discuss your breastfeeding intentions with the staff to be sure they know and understand your expectations, and can help you receive the information and assistance you need. If you plan on breastfeeding, you will need to speak to a staff member about utilizing a breast pump within the first 24 hours after birth. Most hospitals will lend you a pump, if you do not already have one. They can also assist you with the purchase of a breast pump if covered by insurance. A lactation consultant will go over with you how often to pump and where you can pump in privacy in the NICU. While you are pumping for your baby, the NICU should be able to supply storage bottles for your breast milk. Always clearly label your bottles with your child’s name, date, and time. Find out where in the NICU the milk is stored and make sure they are being rotated properly to use the oldest milk first. Try to keep to your pumping schedule in and outside the NICU. By pumping on schedule you can assure your milk supply stays strong and it will prepare you for the schedule of feedings when your child is discharged. When the time comes to breastfeed your child, understand that there can be many challenges to breastfeeding a NICU baby. It’s common for them to tire quickly, have trouble sucking, or become easily distracted. It can all be very frustrating for new moms. Request a lactation specialist to help you with any concerns or problems you are experiencing. Breastfeeding and/or pumping can be a challenge, but it is the best thing you can do for your NICU baby. Remember to stay hydrated and take care of yourself as well. Your milk supply will rely on your well-being.
|


 RSS Feed
RSS Feed