|
Dealing with Insurance Companies
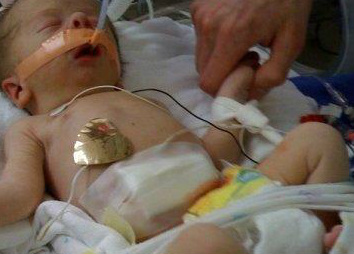
Having a child in the NICU brings with it so many emotions and realities, and often times one of the most stressful ones has to do with medical insurance. It won’t be long before the bills and phone calls start pouring in, and while this is the last thing any new parent has time or energy to deal with, it’s best to be prepared. Here are some tips that might be helpful: The first thing to do is to find your copy of your health benefits book from your insurance company and start reading it over. You most likely would have gotten this when you first enrolled in your insurance plan, and sometimes a new one is given each year with any updates and changes. Find it and start looking at the specific sections dealing with hospitalization charges, specialists, and in network versus out of network charges. You will also most likely have a short window to contact your insurance provider or employer to add your new baby as a dependent. This must be done to be sure they have coverage under your plan. - Contact someone in the hospital’s billing department. They can tell you if they accept your insurance and what your estimated co-pays or out of pocket costs might be for the first couple of days. Sometimes the NICU social worker also helps in this area—be sure to ask. - Start a folder right away labeled with your child’s name and birth date, and keep ALL receipts, notes, forms, and bills in this same folder. This keeps everything together in one place. As a new parent and a NICU parent, your stress level will be high. Don’t add to it by misplacing important papers or forms. Make sure everyone dealing with the insurance knows that all forms go in the folder—it will save lots of headaches down the road. - Keep detailed notes. Whenever you talk to someone about a bill or statement, write down a quick summary of what was discussed. You can do this right on the bill if there is room, or attach another sheet of paper if that works better. Include the name of the person you talked to, the date and time of your call, and a brief summary of what was discussed. This will be helpful if later on you have to talk to someone else about the same issue. -Once the bills start really coming in—don’t stress yourself out by looking them over every day. Just open them, put them in your folder, and designate one day a week to look over them. Nothing is going to change in a week’s time, and by setting aside that specific time each week, you spare yourself a lot of worry and anxiety over each day’s mail. -If you are having trouble paying the bills or not getting what you need, see if your hospital or insurance provider has a medical billing advocate that you can talk to. -Know your insurance company’s appeal process. Sometimes this information is printed right on the bottom or back of bills, if not; check your health benefits book again. If you think a charge is denied and it shouldn’t be, you will have to file an appeal. Often time these are a lot of work—but it is necessary if you think something isn’t being paid that should be. You may also need to get detailed medical records on certain conditions or letters from healthcare professionals like doctors—don’t be shy about asking for these. In this day and age, doctors are well aware of the difficulties found in some insurance policies and most likely will work with you to try and get any issue you may have resolved. -Lastly, find out if you qualify for any state or federal programs. Often, the NCU social worker or discharge planner can handle this. Each state has different criteria and regulations, but you should check to see if your child is eligible for Social Security Income, Medicaid/Medicare, WIC, or any other programs.  Preparing for Discharge Since the time your baby was born you have been anticipating the day that you can all go home as a family. After your baby has completed the necessary milestones, he or she will be ready to go. Although you are elated that this day has finally come, you may also feel anxious to leave the security of the hospital. Try not to worry too much. The hospital staff will help you prepare to take your baby home. They will help you learn how to feed your baby, give medications, take temperatures, and use any specialized medical equipment at home. If your hospital permits, take a chance to ‘room in’ with your baby prior to discharge. This gives you the opportunity to gain experience in your baby's care but have access to nurses if questions arise. The more practice that you are able to get while in the NICU the more prepared you will be when arriving home. Check if your hospital offers infant cardiopulmonary resuscitation (CPR) classes and learn how to administer properly. If the hospital does not offer a class you can check with your local Red Cross or Fire Department. Additionally, make sure your vehicle and home is outfitted with the necessary safety precautions to keep baby safe. Lastly, you may need to select specialists for your baby's continued care. Your baby may also need to undergo routine testing. Make sure to ask your NICU team for this information and see if they are able to refer you to trusted professionals in your area. Staying Organized Congratulations, you are now the parent of a NICU graduate! Right now you are focusing most all your energy on your new baby and trying to understand the overwhelming amount of information that you are being given. Staying organized is a great way for you to gain control in a situation where you may feel you don't have any. Depending on your child's needs you may have several doctors’ appointments to schedule, new medical equipment to learn how to use, and a wide variety of medicine to administer. You need to create a system that will work for you. One of the easiest things to manage is a binder system that is expandable, easy to follow and that you can carry with you. Within the binder you should have a section for all contact information (a list can be found in our contact section), a medication schedule, a section for authorizations that are covered for when your infant has a doctor's appointments, and a place to store information that the doctors provide to you. Also save a place to store your receipts, co-pays, and mileage information as all of that is tax-deductible. Developmental Care Research shows that NICU babies are at risk for developmental delays in speech and language, cognitive skills, and motor skills. Getting these delays identified and treated early gives your child a better chance of reaching his or her full potential. Children that are at risk are often referred to an early intervention program. States are required to evaluate infants and toddlers who are at risk or have developmental delays and disabilities and provide support services to these children. Your child will have a diagnostic evaluation to determine his or her strengths as well as areas that need improving. The evaluation may include health care providers from the following areas: Medical Nutrition Psychology Education Hearing Vision Speech/Language Physical Therapy Occupational Therapy Early intervention programs are designed for families and service providers to work together to ensure the best possible scenario for your child. 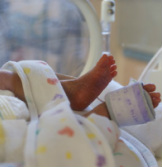 While in the NICU, your baby will be monitored to assess your baby's cardiovascular and respiratory status. The following are common monitoring technologies used in the NICU. Pulse Oximeter - Measures the baby's blood oxygen levels. This technology can be used to detect some congenital heart defects in neonates. Cardio Respiratory Monitors - Three adhesive patches are attached to baby's chest, abdomen, arms or legs. Heart rate, beat pattern, breathing rate and breathing patterns are monitored. Blood Pressure Monitor - Blood pressure is a strong indicator of cardiovascular status in neonates and so should be measured frequently. Temperature Probes - Used to monitor body temperature of neonates, especially when under incubation. Information retrieved from St. Mary's
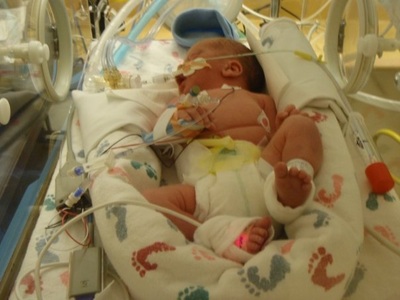
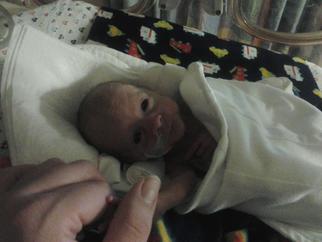 Like most NICU parents we were not expecting to have another premature baby! Losing our first born at 22 weeks was the hardest thing we've ever had to deal with being a newly wed couple, and then 11 months later we got the news we were expecting again. I did everything my OBGYN told me to and at 20 weeks I started dilating again, so emergent cerclage was placed and I lasted 5 more weeks. Brooks was born at 25 weeks weighing in at 1.13 pounds and a whole 13 inches long. That wrinkled tiny guy had my heart from the moment I saw his frail little body. I have never experienced such an roller coaster ride. I remember the day that completely changed my NICU world like it was yesterday! I had just walked into his room when I noticed him not sitting very well, his alarms were dinging and he was not coming back up like he usually did. When all of the sudden it seemed like the bottom dropped out! My tiny guy was BLUE there was several doctors and nurses who kinda pushed me out of the way to get him back where he should be, all of the sudden my little guy vomited all over his incubator, and then it was like he was fine! This happened everyday, and sometimes all day. He was so tired and worn down with all the energy it took just for him to get over his episodes. We finally got the doctor on board to do an upper GI, he got his first trip off the NICU floor. Turns out our tiny guy had stage four reflux. What does this mean? All it means is that, once it goes in it comes out! What can we do for it? Not a whole lot really. All the medicine that could help had bad side effects the main one discouraging me would be death. He was fighting with all his being in the first place and this could or couldn't make it harder for him. So we decided against the meds, we would figure out a way to help him keep his food and everyday meds down. With him still feeding NG and on a pump we decided to slow his feeds down to him taking almost an hour just to eat. It helped a little and shortly after he seemed to be doing a lot better! A whole 107 days we spent in the NICU. We finally were able to go home. He was taking a whole 3 ounces by mouth with the best bottles for reflux I can name, wont name drop but with the initials DB! Today Brooks is your typical two year old! Talking up a storm, getting into everything and anything. At times we still have issues with his reflux, especially if he drinks milk too late. But he is doing very well! Here's to hoping this helps any parents who have had trouble with reflux with your premature angels! 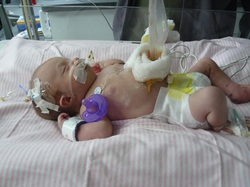 When I went into labor with my first child, I was expecting to give birth to a healthy baby girl. Unfortunately, this was not the case. When our little girl, Hailey, arrived into the world, I heard her cry, but I remember waiting for her to be placed on my chest. When she wasn't and things seemed to be taking too long, I knew something was wrong. I remember looking into my husband's eyes as they welled up with tears and offered no answers, looking as worried and confused as me. Only after our new baby was whisked away to the NICU, without me ever seeing her, did anyone start to explain the situation. It was difficult to focus on the doctor's words, but they began to tell me that it appeared as though she had a condition called gastroschisis. Typically gastroschisis occurs when part of the intestines comes out through part of the umbilical cord. While most cases of gastroschisis occur early in pregnancy and can be discovered during ultrasounds and tests, nothing ever showed that Hailey had the condition. While gastroschisis isn't very common and can be dangerous, it is treatable. Unfortunately to be treated, our daughter had to be immediately flown to a level III NICU hours away so that she could have surgery performed to correct the problem. No one had ever suspected she had any medical issues before her birth and the entire experience of not seeing my firstborn baby after giving birth to her, having her airlifted to a hospital hours away, and then spending time in a NICU because of it was quite traumatic. My husband drove to be with her while I had to wait to be discharged the next day. I was reassured that while her condition and situation seemed quite scary, surgery could correct the problem, and it was likely she would be just fine. When I went to meet my husband and daughter at the NICU the next day, I learned that our daughter had already undergone surgery to place her intestines back inside of her abdomen, and it had went well. When I saw her, it was such an unusual and somewhat scary sight. She had a lot of wires and things attached to her. There was an interesting contraption made out of a rubber band and paperclip attached to her belly that seemed to be helping keep things in place. Unfortunately, this contraption and the healing that needed to occur in her intestines and belly kept us from being able to hold her. While seeing our baby girl like that was extremely difficult, the nurses reassured us that the surgery had went well, and while in most cases they might have been able to say she should recover just fine, in our case, they could not. Hailey began having episodes of apnea where she would stop breathing. They also began to notice other "smaller" issues that raised concern that something else might be wrong with her. And so as she healed from her experience with gastroschisis, the doctors began to run various tests on her. Our NICU experience with our daughter began because of a condition called gastroschisis that could be corrected, but soon our NICU experience changed drastically. Over the next several days, doctors monitored Hailey as she healed from surgery and ran many tests on her to try to find a diagnosis. Her gastroschisis, apnea episodes, and other signs like a skin tag and what they considered small set eyes, led doctors to believe she might have another condition that eventually caused them to run a FISH test (Fluorescence In Situ Hybridization). It took several more days to receive the results from that test, but when they came back with the results, nothing could have prepared us for what they were about to tell us. The doctors told us that the results showed that our daughter had Full Trisomy 18, a lethal genetic disorder that meant she had 3 copies of her 18th chromosome, instead of the normal 2, in every single cell of her body. This prevented her body from functioning and developing correctly. They told us that her form of Trisomy 18, Full Trisomy 18, was caused spontaneously at contraception, was untreatable, incurable, and fatal. The doctors couldn't tell us how long Hailey had to live. They explained it could be hours, days, weeks, maybe months at best. Because of her frequent apnea episodes, they felt it could happen any moment.In light of the learning our daughter had Trisomy 18, we were then faced with decisions no parents ever expect to make. We also learned a lot of information about Trisomy 18. Some from our medical staff, but mostly from our own research online. We learned that Trisomy 18 affects babies differently and there are different types of it. Most Trisomy 18 babies die in utero or are stillborn. Those who do survive birth are unlikely to make it to see their first birthday. Unlike most Trisomy 18 babies, Hailey's major organs were healthy and functioning (the only problems she had were in regards to her apnea and poor breathing). Many babies with Trisomy 18 have heart and / or kidney problems, they also often have cleft lips, but she had none of those. She really seemed like a healthy baby who only had gastroschisis, but a closer look proved otherwise. The other signs, like I already mentioned, were cosmetic, like her skin tag and small features. But because of the frailty of her life and many other factors, we made the difficult decision to stop medical intervention so that we could hold her and cherish our time together as a family. The hospital staff released us from the NICU and moved us to a private family room in the hospital where we stayed for a few more days while doctors and nurses monitored her. We held her constantly and were able to spend time bonding with her. She always wore a nasal cannula to help her breathe, and she worked her way from receiving IV nutrition and a feeding tube to taking breast milk from a bottle, which was an incredible milestone. Eventually Hailey was stable enough and receiving enough nutrition from a bottle to be able to leave the hospital and take her home with us. We were in the hospital with Hailey for almost a week and a half, displaced hours away from our home, and hundreds of miles from our families (my husband is in the Army, and we were stationed very far from our families). Thankfully our families were able to fly and be with us while we went through this traumatic time. When we came home with Hailey, hospice care was provided to us. A hospice nurse came every day to check on her and us. At home Hailey had a nasal cannula and oxygen tank, a feeding tube we were taught to use if she began to have problems with the bottle, as well as pain medication, and we monitored her closely. We spent our days at home holding her as much as possible. After over a month, as doctors predicted would happen eventually, our sweet girl developed an infection that quickly ran through her body and caused her to pass away after about 24 hours of its onset. Our daughter Hailey lived for 36 days. While Hailey was alive and after she died, our faith in God provided us with strength to carry us through the days and allowed us to see the blessings in the darkest time of our lives. We found additional comfort and support through our family and friends, through online child loss groups, and through sharing our family’s story. Additional note: Trisomy 18 can be diagnosed when the baby is in the womb; however, in our case, screenings missed it. We had a genetic screening done early in my pregnancy with Hailey. Part of the screening suggested she had a slight increase of fluid behind her neck which may be an indicator of a chromosomal disorder like Trisomy 18, but not always, and the other part of the screening which required blood work came back normal, which suggested she did not have a disorder. With the two results of the screening together, the doctor determined her screening was negative for a chromosomal disorder, and that proved to be incorrect in the end. Written by: Kristin Vanderlip, Division Coordinator of Hailey's Hope with Project Sweet Peas.
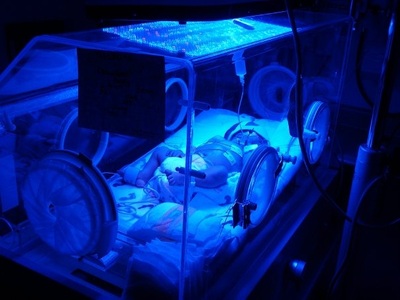
Jaundice is the most common complication seen in newborn infants. It affects both full-term and premature babies, usually appearing during the first week of the baby's life.
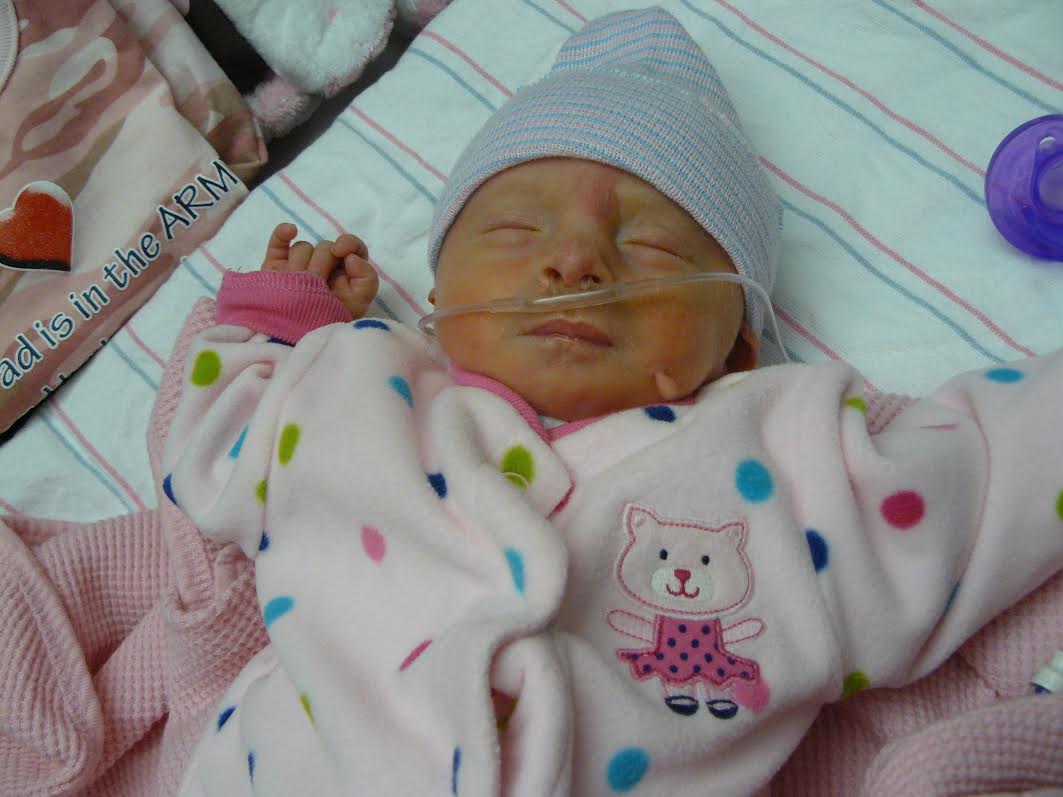
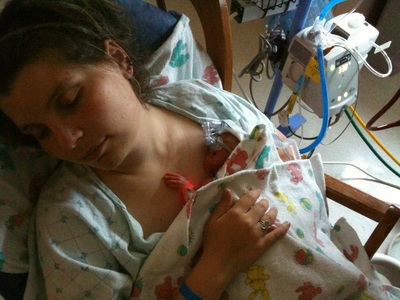
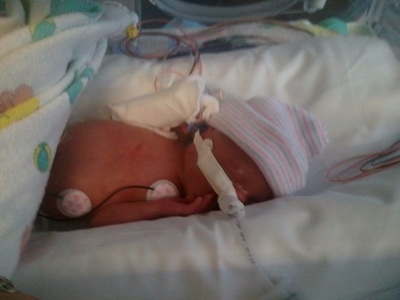
Born 7 weeks early. Stephen was intubated, suffered from jaundice, reflux and dropping heart rate. Due to the severity of jaundice, he required phototherapy. Phototherapy is the process of using light to eliminate bilirubin in the blood. Stephen spent 19 days in the NICU and was released right before Christmas. He joined his twins sisters at home, where they are all growing happy and healthy. It is funny how you don’t really want something until you can’t have it, and then that is all you want. I never thought of myself as a “Mommy” person; don’t get me wrong, I loved kids, but I used to tell people I was too selfish to have kids. It was only after I was told that because of an issue with severe anemia, I probably was not healthy enough for kids, that I wanted nothing more than to be a mom.
In November 2011, I woke up feeling “off”. I didn’t feel sick; I wasn’t depressed, I just felt different. A friend of mine suggested I take a HPT. I knew the results would be negative, so I was shocked when 2 pink lines appeared almost immediately. But that is also when the numbness hit. Part of me was excited that there was a possibility I would be a mom, but there was also an even bigger part of me that said, “Don’t get your hopes up; your body is not healthy enough for a baby.” After talking with my boyfriend, we decided to keep the baby a secret until we were out of our first trimester, both feeling like there was a huge possibility we would lose it. Once I hit 13 week, I went in to the local pregnancy center (at the time I was without insurance) and heard the most beautiful sound in the whole world, a nice, healthy beating heart. I know it sounds cliché, but hearing MY baby’s heartbeat, made it all real, and I began to feel a love I had never felt. Because of insurance problems and other unforeseen issues (like finding a doctor) I didn’t get in to see my OB until my 22nd week. He listened to the heartbeat, took some measurements and scheduled my anatomy sonogram. He gave me a small lecture about waiting too long, but said with a smile, “Your child seems healthy and you look good, so I think all will be fine.” Many times people asked me when I was pregnant what I wanted, and I always responded, “I don’t care, as long as it is healthy”. It was only after Shiloh’s birth, that I began to cringe at the thought of that statement. Did I want my daughter any less because she wasn’t healthy? If anything I loved her more, because I had watched her struggle and almost leave me, and then come back fighting with a will to live that I could only dream about having. On April 24th, I went in for what I thought would be a normal sonogram. As the tech was moving the wand over my belly, she was pointing out all the body parts. At one point she asked, my daughter's father, Graham and me if we would like to know the sex. She then told us that we would be having a baby girl. I was so excited; I didn't think anything could pull me down, but I was wrong. The next thing she told me still makes me cringe today. She got really serious, and said that she would be sending me to labor and delivery, because something didn't look right. To say I was scared is understatement; all I could think about was how I did not want to lose this little girl I was madly in love with. Once in L&D, the nurses explained that I was dilated to 2 centimeters and that the amniotic sac was bulging through my cervix. They did a fetal fibronectin test to see if I was at risk for preterm labor- after about an hour they came back and said that the lab was backed up and that they could not get the results. Since I had an appointment with my OB the following day, they told me to go home and stay off my feet until the next day and we would go from there. The following morning, Graham and I went to meet with my OB, Dr. Mills. He told is that after getting the results of the FFN test and seeing the sonogram that I would need to go immediately back to L&D, most likely for the remainder of my pregnancy (At this point I was only 24 weeks). He followed us over there and after another exam told me I was now dilated to 3 cm, and that I had what was called an incompetent cervix. He went on to say that most of the time when it is caught early enough they can do a cerclage and close the cervix, but because I was now dilated so far, so quickly and the fact that my amniotic sac was bulging, I was clearly not a candidate. The good news was, I was far enough along that my daughter was viable, but the bad news was I would probably not make it to 30 weeks. The following morning I had another sonogram that pretty much said the same thing Dr. Mills had been telling us, so I was started me on betamethasone to mature baby's lungs, and then magnesium sulfate to mature the brain to reduce the risk of neurological issues. Because of Dr. Mills' fear that I would probably go into labor soon, I was transferred to UC San Francisco Benioff Children’s Hospital, which had a high level NICU (my current hospital had no NICU). It was then that it all began to sink in. I knew this was really happening. I was most likely going to give birth to a premature baby, and like all parents this was not in my birth plan. Over the next 2 weeks, I was given many tests, talked to many doctors and each day felt worse and then better at the same time. I knew all of the “bad” things that could potentially happen, but I was hopeful that it would all come out relatively ok. I talked with neonatologists that explained the development of my daughter, and was given a tour of the NICU to see what other babies looked like born at different gestational ages (But nothing truly prepares you for a premature baby). During the night on May 5th, 2012, I got up to go to the bathroom and just as I stood up, water gushed out of me. I knew there was no holding back then. I called my nurse, who came in and confirmed that, yes my water had broke. And that there would be nothing they would do to stop my labor. Over the next few days everything was a blur. I was depressed because she was on her way and I felt I had failed. Maybe if I hadn’t got up so much, maybe if I had been more careful, every what if ran through my head. Then on top of that I was on high doses of erythromycin, which I was allergic to, but continued to take because I wanted my daughter to come out as healthy as possible. On May 7th, the contractions started, and I knew that my little one would be arriving soon, I knew that I was at the finishing line of my pregnancy, and that the real scary stuff was about to happen. I think I did more praying that I had ever done in my entire life. By 6am the next morning my contractions were so bad that I gave in and got an epidural. I was told I was still only dilated to 3cm, but I guess the epidural was what my body needed to relax, because at 8am when the nurse came in to check me, my daughter’s head was almost out. I was rushed into the delivery room, and two pushes later my daughter, Shiloh Marie was born. My only glimpse of her was when they cut the cord. She looked purple and tiny, but did let out one small little breath, so I knew she was going to be ok. Shiloh was born at 8:21am, May 8th 2012, weighing 2.3lbs and was 14.5 inches. She was covered in platinum blonde hair and had the most beautiful eyes I had ever seen (she still does.) My official medical reason for giving birth early was Sepsis and PPROM caused from an Incompetent Cervix. But in all honesty it was worth it to have such a wonderful little creature. Our NICU stay was for the most part uneventful. She was there to grow, learn to breathe and eat. We went through all the normal stages. High Flow Vent, CPAP, nose cannula, by 4 weeks old she was breathing completely on her own. She was good at tolerating all her NG feeds and maintaining her body temperature. We believed we would be going home well before her intended due date, but as any mom can tell you, children are very unpredictable. On Thursday, June 21st, I walked into the NICU to a very noisy room, and the sound of every alarm on Shiloh's monitors going off, but before I completely freaked, I decided to check on her to hoping that is was just a machine malfunction. As I walked to her crib I notice my baby girl was ashen blue and was not breathing at all. Of course I immediately began to freak out. I tried to stimulate her in hopes that she would take a breath, fearing that my little girl was already gone, and yelled out to the nurse that my baby was blue. The nurse came running, tried to suction out her mouth, and then said the words I was hoping I wouldn't have to hear, "Get her team in here, we have a code blue". I ran to the hall and watched as a team of 7 people rushed to my baby's bed. I then leaned against the wall, praying like I had never done in my life, just saying over and over, "God, please do not take my baby girl, I will do anything just don't take her". About 30 seconds later I heard the most beautiful sound in the world, my little baby, crying. The charge nurse came out, and told me I could go in and hold her, but she had aspirated on some formula, and would probably need some breathing support. As I held my little Monkey, I felt a love that I have never felt before (don't get me wrong, I have loved her so incredibly since the second I found out I was pregnant, but after feeling like I was going to lose her, my love only grew stronger). To feel her tiny breath against my cheek, to hear her baby cries, I felt like I was given a second chance and I guess in a way I was. Then the questions set in. How long had the alarms been going off? Even though it was a little noisy, why had neither one of the nurses heard her alarms? And the worse question, what would have happened if I hadn't walked in when I did? After x-rays, we found she had collapsed her left lung and would most likely have pneumonia. She was put on a ventilator and was given morphine for the pain. It was then in it all hit me again. My 6 week old baby girl, who had been healthy since the day she was born at just a little over two pounds, now had a collapsed lung and pneumonia, because of a careless mistake. I sat there, crying again, feeling helpless. Wanting nothing more than to wrap her in my arms and hold her, knowing that I couldn't because she was on so many tubes, and had multiple IVs. I just sat there staring at her swollen body, hoping she wasn't in too much pain. It was then that Graham and I had a chance to actually sit down and talk to her doctor. He told us that she would be getting antibiotics to help minimize her pneumonia, and that, because she probably only went without breathing for 3-4 minutes, and that she still had a heart beat, she most likely would not have any brain damage. But because of the degree of aspiration she might have lung damage. And then the only thing I didn't really want to hear, had I not walked in when I did, she would have probably died, that as helpless as I felt at that moment, I had actually saved my baby's life. It was a couple more weeks before we were told that Shiloh did in fact have some extensive lung damage. Her left lung was complete scar tissue and she would most likely deal with lung issues for her life. I will not lie, I was angry, but at the same time I was okay knowing that this was just one for hiccup in the road. My daughter was alive and she would be okay, she was beyond strong! We were finally able to leave the NICU on Aug 9, 2012, after 94 days, and 2 days before her due date. She left on oxygen and an NG tube (because she didn’t have the energy to eat anything). She remained on O2 until the following January, and the feeding tube until September. Over the first winter she got RSV twice and the second winter once (all mild cases, due to receiving syngis shots), but continued to get healthier and healthier. Now Shiloh is a extremely spirited little 2 year old that enjoys Batman and Mickey Mouse Clubhouse. By looking at her you would never know that she once spend 3 months in ICU after coming in this world 3 months early. And as cliché as it sounds she is the best thing that ever happened to me, my tiny miracle. As for future children, it is still something I think about. I have researched different kinds of cerclages, and things I could to better my chances of going to term. But in all honesty, I am not sure I could do the whole NICU experience again. It changed me and how I look at things and definitely made me, sometimes, too overprotective to my little girl. But only time will tell. 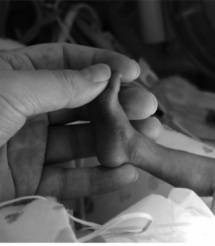 Although every premature baby's story is different, below are some common prematurity complications. Intraventricular hemorrhage (IVH): IVH is bleeding into the fluid-filled areas (ventricles) inside the brain. Prematurity (and the degree of prematurity) is a risk factor for this condition. There are four grades of IVH. Grades 1-4 indicate severity of the bleed. Learn more at NIH. Hydrocephalus: Hydrocephalus is a condition in which excess fluid accumulates in the brain. This causes widening of the ventricles and can put pressure on the brain. A common treatment for hydrocephalus is surgically placing a shunt system in the brain to rid the brain of excess fluid. Learn more at NIH. Periventricular leukomalacia (PVL): PVL is a disorder in which there is a death of white brain matter caused by lack of oxygen or blood to the periventricular portion of the brain. There is no treatment to cure this condition. There are only treatments to alleviate symptoms. Learn more at NIH. Bronchopulmonary dysplasia (BPD): BPD is caused by prolonged periods of high levels of assisted ventilation. Congenital heart disease, prematurity and severe respiratory infection are risk factors for BPD. Infants with this disorder may be fed by NG tube and require extra calories. Diuretics, corticosteroids, bronchodilators and surfactant are common medicinal treatments. Apnea: Apnea is caused by immaturity in the area of the brain that controls the drive to breathe or by illness. Intraventricular hemorrhage, intracranial hemorrhage, neonatal seizures, perinatal asphyxia,, Impairment of oxygenation from congestive heart failure and pulmonary edema (PDA, coarctation, etc.), or from shunting (cyanotic heart disease) are common risk factors. Persistent Pulmonary Hypertension (PPHN): PPHN occurs when there is a failure of the normal circulatory transition that occurs after birth. Risk factors include meconium aspiration syndrome, pneumonia, infection, low blood sugar, birth asphyxia, amniotic fluid leak and low amniotic fluid. Treatments include ventilation, nitric oxide, and ECMO. Pneumothorax: This disorder occurs when alveoli in the lung burst which leads to leaking air into the pleural space. RDS and meconium aspiration are causal factors. This condition is treated by placing a catheter into the baby's chest to remove the air. Respiratory Distress Syndrome (RDS): RDS occurs when an infant's immature lungs do not produce enough surfactant. Ventilation and surfacant are common treatments. GER disease (GERD): occurs when reflux of the gastric contents causes symptoms that affect the quality of life for an infant. The predominant cause of GERD is transient lower esophageal sphincter (LES) relaxation. Regurgitation and vomiting are the most common symptoms of infant reflux. In GERD, the reflux contains stomach acid which damages the lining of the esophagus. Feeding changes may be necessary. Medication and surgery may be necessary dependent on severity. Learn more at NIH. Hypoglycemia : This condition occurs when a neonate has low levels of blood sugar. Glucose blood levels can drop in neonates for the following reason:
Patent ductus arteriosus (PDA) : PDA is a condition in which the ductus arteriosus does not close. PDA leads to abnormal blood flow between the aorta and pulmonary artery, two major blood vessels that carry blood from the heart. Surgery may be necessary if the PDA does not close on its own. Learn more at NIH. Jaundice: is the most common condition seen in newborns. It occurs when high levels of bilirubin are exhibited in the blood. This causes yellowing of the skin. In extreme cases fatigue and poor feeding are seen. In mild cases treatment might not be necessary. The condition is simply monitored. If bilirubin levels are very high, phototherapy may be required to break down the bilirubin (as pictured). Rare complications include deafness, cerebral palsy and kernicterus (brain damage). Learn more at NIH.  Gastroesophageal reflux (GER) occurs when there is an involuntary retrograde passage of gastric contents into the esophagus with or without regurgitation or vomiting. GER disease (GERD) occurs when reflux of the gastric contents causes symptoms that affect the quality of life for an infant. The predominant cause of GERD is transient lower esophageal sphincter (LES) relaxation. Regurgitation and vomiting are the most common symptoms of infant reflux. In GERD, the reflux contains stomach acid which damages the lining of the esophagus. Feeding changes may be necessary. Medication and surgery may be necessary dependent on severity. Learn more at NIH. Information retrieved from NIH and the Mayo Clinic
|



 RSS Feed
RSS Feed