 Dads have such an important role in the NICU, but at times it can seem as if your role is secondary, as everyone around focuses on Mom and her recovery, needs, and emotions. Don't let this discourage you. Your role and support is vital to your baby's well-being. You may find yourself feeling helpless and at a loss as to what to do. Strong and often contradictory emotions, such as anger and sadness, guilt and grief, helplessness and hope may be swirling through your head throughout the day. Stop and take a moment to acknowledge what you are feeling and just how difficult your situation is. Having a child in the NICU may be the hardest thing you ever face in your life, so now is not the time to try to do it all. Focus on what you can do to help yourself, your baby and your partner. Helping Yourself Taking care of yourself physically and emotionally can be a challenge while in the NICU but you'll be better prepared for your baby's care if you are at your best.
Helping Your Baby Looking at your new baby hooked up to machines, looking so small and frail....this is not what you imagined fatherhood to look like. You may be extremely nervous about holding your baby, and participating in his/her care for fear of doing something wrong. Pay close attention to what the nurses are doing and ask lots of questions so you can feel confident about helping. They know that all parents are nervous about what to do, so no question will surprise them. Take notes if you need to or have them stay right there with you the first few times until you feel comfortable. The most important thing is not to the let opportunities pass you by. You will want to experience and remember these special moments. Learn more about staying involved in your baby's care here. Helping your Spouse or Partner You may find yourself wondering just how Mom is able to handle everything -- and the secret is, she can't do it without a lot of help. Make sure you are helping take care of her so she is able to focus on your child as well. Some things that might help:
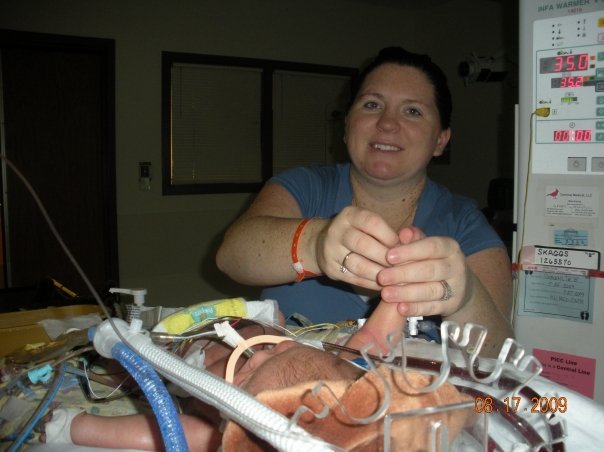
Most of all, try to take one moment at a time and enjoy special moments and milestones with your family. Your baby has had a rough start to life and you have an integral role in her/his care.  Parental involvement in baby's care in the NICU is important for both the health of baby and his or her parents. Although the experience may be overwhelming, you play an integral role as an advocate and voice for your child. Below are 7 ways that you can stay involved in your baby's care. 1. Ask questions and take notes - No question is too small. This is your child and staying informed is important. If no one is around to answer, write down questions you come up with to ask later. If you are even the slightest bit concerned about your child's condition, ask questions! The nurses and doctors are there to help you understand and make informed decisions in your child's care. To help you remember the answers to these questions and to record your observations, keep a journal. It can be a great tool to refer back to later on. 2. Know your nurses - Every nurse is different with a unique personality, routine, and opinion. If you have a primary nurse, make sure you dedicate time to connecting with him or her. Your primary nurse is charged with your baby's plan of care and will be a resource to you throughout your stay. If you don't have a primary nurse, inquire to see if one is available. 3. Make Sure Your Expectations are Understood - Most parents have a preference on the parenting style and care that they chose for their child. Breastfeeding vs. Bottle, the use of pacifiers, religious considerations, etc… are all topics that should be discussed. Keep an open mind, not every request may be able to be accommodated based on your child’s condition. However, by informing the staff of your wishes, they can help you make the best decisions for your child. 4. Know the Routine - A NICU has a specific routine in place. By knowing the routine you can be better prepared as to what to expect during your stay. Find out how long the shifts are, and what time shift change takes place. Ask what time rounds are made, and if you are allowed to be there during these times. 5. Know the Rules - Each NICU is different; all rules will vary depending on the hospital’s policy and the severity of your child’s condition. Most NICU’s will hand out guidelines, but if not, make sure you check on a few things the first day. For example: What are visiting hours? How many people are allowed at your child’s side at a time? Are physical interactions such as bathing, diapering, feeding, and holding your child, limited? Can you bring items in from home such as a book to read to your child, or stuffed animals and pictures to leave in the isolette? What phone number can you use to check on your child? 6. Be present as much as possible - interact with your baby as much as permitted by your NICU. Your baby knows you as his or her parent and so will feel comfort from your presence. Advocate for Kangaroo care and other bonding practices when your physician feels your baby is stable enough. Inquire to see if you can participate in bathing your baby, taking his or her temperature, changing diapers and other care procedures. Remember that although being present for your baby is critical, you should also make sure to take care of yourself. You'll be better prepared for your baby's care if you are at your best. 7. Celebrate the milestones - There are many different ways to celebrate the milestones of your baby. From journaling and scrapbooking, to stickers and journey beads; you will want to capture the moments that bring your baby one step closer to home. Don’t forget to take pictures. Many parents are reluctant to take pictures of their critically ill newborns, but this is an important time in their life that you will want to document to see just how far they’ve come. Keep in mind that all babies are different and your child’s milestones may not follow the typical timeline. Discuss your concerns with your child’s doctor and try to be patient; your little one is working hard to overcome the additional obstacles he/she faces to get there! Seeing your unborn child, the flickering movement of his beating heart and already active hands and feet on the ultrasound screen is magical. A moment in time that is always impressed on your memory. On September 2, 2008 my husband and I found ourselves enraptured in that moment – overwhelmed with the pure joy of seeing our first child on that screen. The ultrasound technician took his time and pointed out waving hands, eyes wide open, and feet that would not sit still. He sent us back to the waiting room with a flimsy printout in hand of the most perfect baby profile – complete with tiny turned up nose that we lovingly quipped as very elf-like. Next to the moment of getting that positive pregnancy test after nearly two years of trying to conceive, this was the most joy-filled, heart-swelling moment we had experienced. We gushed, took pictures of that amazing little profile with our phones, and sent our love and joy along to our family and friends while waiting to be called in for the rest of our appointment. We were called back and ushered to an examining room where we eagerly showed our little picture off to the nurse. She gave her obligatory “oohs” and “ahhs” and let us know that Rita, the physician’s assistant I had seen regularly through my pregnancy and had known since I became a patient of this office at 18, would be in shortly. We waited. And we waited. And we waited some more. Finally, Rita came in and in my excitement to show her the cutest turned up nose ever, maybe I missed her air of worry and impending bad news. “We think there’s something wrong with the baby.” Those eight words changed my life the very second they were uttered. The ultrasound technician believed he saw a diaphragmatic hernia, but we would be sent to the Regional Perinatal Center to receive a definitive diagnosis. It could be nothing, she said. But I knew. And my heart sank. The soaring high of falling in love with my baby on screen followed by the screeching halt and plummet into the unknown was more than I could bear and I fell apart. Rita assured me that we would be in the best of hands and there was no use in worrying yet and she hugged me as I cried in that examining room. We were scheduled for an appointment at the Perinatal Center the following week. We were warned it would be a very long and strenuous day, which was an understatement at best. The waiting room was loud and void of anything happy or pleasant. Women and families from every walk of life in all stages of pregnancy filled the waiting room seats. With my husband at my side, holding my hand tightly, we found ourselves waiting again. We were eventually called back for our ultrasound and I lay there in silence watching my sweet baby up on the screen, praying for the news I knew in my heart we wouldn’t receive. Every question we asked was met with the same answer – that the doctor would speak with us about the results afterwards. After spending more time in the waiting room and then in a generic, sparsely furnished office, we finally met with the woman who held our answers. She confirmed our diagnosis and asked us – a teacher and an engineer, who she assumed had already scoured the internet – what she could tell us. While we had let Google fill our minds with facts we would rather not hear, we asked her to just tell us it all. We needed to hear it from her. In short, Congenital Diaphragmatic Hernia (CDH) means that the diaphragm of our baby failed to form completely in utero, thus allowing the baby’s abdominal organs to migrate and grow in the chest cavity. This in turn causes for poor or no lung development and pushes the heart out of place. Overall, the defect carries a staggering 50% survival rate, though she did think our odds were greater. Other defects can be linked to CDH, but there were no obviously glaring issues presenting (and we opted to not have additional testing done as it would not have changed our course of action at all). CDH babies are typically among the sickest in the NICU and can require the highest means of life support to get them through. She reassured us that Crouse Hospital, where we planned to deliver, was an excellent choice in hospitals and they were well equipped to handle a baby such as ours. I and our baby were to be closely monitored for the rest of my pregnancy and we would be scheduling appointments to meet with the pediatric surgeon, who would eventually correct our baby’s defect, and a neonatologist from Crouse, who would give us a run down of what to expect and take us on a tour of the neonatal unit. Our first true NICU experience – this meeting with the neonatologist – was a tough pill of reality to swallow. It seemed as if the resounding opinion of people we talked to in general was that at least we knew what we were in store for – we could prepare and not be bombarded with the experience with no forewarning. We went into this meeting brave, yet apprehensive – trying to embrace this thought that knowledge is power. But, really, a stone-faced doctor telling us that as soon as our baby is born he would be whisked away by a medical team to be stabilized and placed on a ventilator, so don’t expect to get to hold him crushed me. I was not naïve; I knew this was bound to be our reality. It didn’t make hearing that reality any less painful. We followed this meeting by taking a quick tour of the NICU where we were told the practices and policies we were to follow as patients there – diligent hand washing, signing in and out, limitations on who would be allowed to visit and when. More information to add to our already spinning heads. Walking through the NICU was a sensory overload – the sounds and smells and sights and general buzz of energy filling those crowded hallways and nurseries was almost more than we could handle in that moment. We went home dejected and overwhelmed. Our beautiful son, Charlie, came into this world on his due date, February 4, 2009 at 9:52pm, weighing 7 pounds 11 ounces. My midwife held him up, announced he was a boy, and I saw him for the briefest second before he was handed over to the team of doctors and nurses from the NICU waiting for him. I had the passing thought that he wasn’t crying, though I rationally knew he wouldn’t. My husband had moved to the other side of the room where they were working on Charlie and was trying to take pictures past the multiple people surround our tiny boy. He had been born fighting. It took six people to hold him down to intubate him and get an IV started with medication to sedate him. They paused for the briefest of moments to allow our deacon to come into the room and baptize him before whisking him out to the elevator, the doctor calling over his shoulder to give them time to stabilize him and get him settled before coming up to see him. By the time Charlie was stabilized and I was able to get out of bed and move off the labor and delivery unit, it was nearly 3 in the morning. A nurse rolled me into the subdued middle of the night NICU with Vince at my side. Our Charlie was in Nursery C taking up almost two bed spaces with all his equipment and a nurse dedicated to taking care of him and him alone. He was hooked up to an oscillating ventilator that made a nonstop racket and shook Charlie’s small body. There were wires and tubes and monitors and numbers flashing that I did not yet understand, but would come to know as well as the nurses themselves in the coming weeks. All of this going on around him and I honestly saw none of it. All I saw was my sweet little boy. His soft dark hair. His little upturned nose. His long delicate fingers that he readily wrapped around my finger. I was lost in him. I didn’t cry. I was not afraid. In that moment it all seemed right. His nurse, who at first glance seemed rough and tough, gently explained that NICU babies needed strong, firm touch – not light, feathery caresses that could send them into a sensory overload. She showed me how to wrap one of my hands firmly yet gently around his little bare feet and the other around his tiny head. I was in love. The next day we met our NICU angel – Charlie’s nurse, Dee. She was with him for 12 hours that first full day and was an immediate comfort to us. She put us at ease, made us feel like we could ask questions. We felt comfortable being at Charlie’s bedside and never like we were in the way when she was there. She took our family on as her personal cause and she championed us through our journey – laughing with us, crying with us, and seeing us through the rollercoaster that is the NICU. My third night on the postpartum floor, the night before I was to be discharged, I woke to pump as I had been doing religiously every three hours. Sitting in bed in the dim light, with the constant whoosh whoosh of the hospital grade pump, not thinking of anything in particular, I heard from the hallway someone walking past my room with a crying baby and I suddenly lost all sense of the calm and peaceful front I had been putting up. Without warning I could feel my throat closing as I tried unsuccessfully to hold back the wash of emotions that I was suddenly drowning in. Vince, who was sleeping on a small pull out couch next to me, woke to my gasping, choking sobs. The reality of what my baby laying two floors above me was going through hit me like a ton of bricks. But even harsher perhaps was the reality that the next day I would be going home and leaving him there. I knew that leaving that hospital empty handed was going to tear me apart. I would be leaving a piece of me, a piece of my very heart and soul, behind. There is nothing that can make that ache bearable. On Charlie’s sixth day of life, he was deemed stable enough for surgery, but not so stable that the surgeon felt comfortable actually moving him. It was decided that they would bring the operating room to him. We stayed by Charlie’s bedside while they moved in equipment and tools and people who did not fit easily in that space. As we started our reluctant move away from Charlie’s side, Dee came over and put her hand on my back and said, “Give your little man a kiss on the head.” I had not kissed him before this and my eyes filled with tears as I laid my lips gently on the top of his head and whispered my infinite love for him. We waited in the hallway outside the NICU doors watching parents come and go, wondering what their stories were. The hallway itself was full of stories – framed with pictures and given to the NICU by families whose lives had been changed behind those double doors. Some stories had happy endings, babies beating the odds no matter how high they had been stacked against them. Some stories ended in ways no parent would want to imagine. But the overwhelming theme was the intense love and respect these families had for the doctors and nurses and various other people who gave of their time and talents in this NICU. Those words were our comfort. They showed the path that had come before us and we vowed to add our own story to those walls someday. Charlie made it through the surgery and progressed in typical NICU fashion over the next days. There were good days and there were not so good days. The NICU rollercoaster is a very real thing. We learned to take it one day at a time and really tried to just keep our spirits up. One evening in particular we sat next to Charlie’s bed not being able to do much but just sit there. His numbers were not great and we knew not to bother him for fear of making matters worse. It was not the happiest of places we had been, but Vince started cracking corny jokes to lighten the mood. Our nurse and others in the room snickered at his wise cracks and before long our nurse pointed out that Charlie’s number slowly, but surely were improving and she encouraged us to just keep doing what we were because it was obviously working. The NICU was most certainly a serious place and with good reason to be so, but we learned that night that maybe laughter has its place there as well. Charlie continued his dance on the road to his eventual recovery – ventilators were switched, settings tweaked, chest tubes placed, medications added and weaned. When he was three weeks old, I was in my usual chair next to his bed, helping with his care when I could, and Dee asked if I wanted to hold him. What?! Part of me wanted to scream “Yes!” and run and get the nearest sterile gown, but part of me wanted to slam on the breaks and make sure this was really a good idea. Dee reassured me that it was time and that both Charlie and I needed it. I asked if we could wait until Vince got out of work and just about bubbled with excitement until then. There are no words for the sheer volume of emotions I went through sitting in the rocking chair with him in my arms, ventilator tube taped to my shoulder, and staring into his alert little eyes. Another moment in time, etched into my memory. The days and weeks progressed and Charlie was growing and improving in leaps and bounds. He was successfully taken off the ventilator and transitioned to a low vapotherm support, he was weaning off his pain medications without side effects, he was tolerating feeds via NG tube well. It seemed like we were on the right path, sailing through towards the finish line. And then we were faced with “the episode” – this is what our doctors referred to it as since they had no other words. It was Monday, March 23rd, and it was bath day in his new progressive care nursery. Our nurse was Lynn – she had taken care of Charlie many times when he was at his sickest, had even assisted with his surgery. She did not typically work with babies once they were moved to progressive nurseries, but this day she was. I helped Lynn bathe Charlie – a sponge bath in bed because he wasn’t allowed to be submerged yet due to his PICC line. He screamed and fought us, which was common for him. And then he stopped. And he turned purple. And he went limp. And I have never been so scared in my entire life. I backed away from his bedside not even aware of where I was going as the doctor rushed into the room. Another mother in the room came and put her arm around my shoulder and stood with me as we watched them frantically resuscitate my baby boy. I asked a nurse nearby if I should call my husband and she directed me to the phone. I had just been holding that sweet boy in my arms, singing him lullabies and now…. I couldn’t reach my husband right away and when I did I struggled to explain what was happening. He rushed to join me at the hospital while others looked at me sadly and rubbed my back as I stood at his bedside where he lay so pale, sedated and on paralytic medications once again as the ventilator breathed for him. I was broken. How could I ever trust that he was well if things could turn on a dime with no warning? Someone came and told me I had a phone call – another nurse had called our angel Dee at home on her day off and she was calling to comfort me over the phone as she also cried for the trauma we all suffered that afternoon. In the end, tests were run, specialists were consulted and no one could put a finger on what had happened for sure. I suppose what is most important is that he recovered. He came off the vent within a few days and rebounded coming off even vapotherm within days after that. But I struggled to push that cloud of worry and doubt away. Thus is the life of the NICU mother, I suppose. Perhaps the most difficult moment to explain came at the end of our NICU journey. April was drawing to an end and it became clear that the team of doctors and nurses who had brought us from day one to here were ready to set us free from the hour walls of the neonatal intensive care unit. One would think that revelation would have brought me overwhelming joy, but instead I felt an insane level of fear and trepidation. The NICU was our safe haven. What if something happened? That anxiety has never left me. It has certainly quieted over the years, but I always have that nagging worry in the back of my head that things could go horribly wrong when I least expect it. The other side of my less than excited feelings towards Charlie’s discharge were tied to the people we had met along our journey. There were other parents who lived hours away but we became comrades and friends while our babies grew together in little hospital grade beds. No one can understand what it is like to be a NICU mother or father unless you have actually been there. People can try to sympathize, but they just cannot know. There is no way to understand without those first hand, heart breaking experiences shaping you. And then there’s the nurses – how could I begin to thank those people who literally saved my baby’s life and taught me how to be a parent while they were at it? It takes an incredibly special person to do what they do every day and to do it so well. They too became my friends. I knew I was going to miss them horribly once home. Don’t get me wrong, going home with our miracle boy was amazing and almost more than I could have hoped and prayed for. I just never realized how much I would miss the life I had made in the NICU. After 85 days in the NICU at Crouse Hospital, my Charlie came home. Today he is an amazing five and a half year old little man. He is happy. He is healthy. He is a big brother to an equally amazing (and healthy) two year old sweet heart of a boy named Bennett. He has made me who I am today. Each of those 85 days and the bumps and bruises and the joys and elations they brought have changed me. I am a better person for all we endured. My husband and I have said numerous times to many people, if we were given the opportunity to go back and do this all over again, we would not change a moment. And I mean that from the very bottom of my heart. 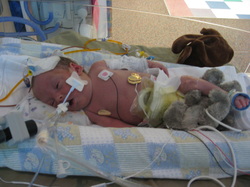 Three years ago, we began our journey as parents to a child who went to heaven and a child who stayed here on earth to fight for his life against a rare disease. It has been the toughest thing we have ever had to do. This is our story . . . I remember February 10, 2011 like it was yesterday. I was nearly 31 weeks pregnant with two perfect, healthy identical twin boys: Kaysen Preston and Tysen Lucas. The events that happened that day and the months afterwards constantly replay in my mind. Because I was pregnant with identical twins I was monitored closely with weekly ultrasounds. On February 10th, I went in for a routine ultrasound. Both babies had been rambunctiously moving around all morning, so as I lay there on the ultrasound table, I was thinking about where I would be eating lunch and had no reservations about the appointment. Even when the ultrasound technician left the room and came back with the doctor, I thought nothing of it. Thirty seconds later, my safe, happy, carefree world was turned upside down. I will never forget the words that came out of the doctor’s mouth: “I’m sorry, but Baby A has no heartbeat”. I was so confused. I had JUST felt both of them moving. What did he mean he couldn’t find a heartbeat?! He went on to tell us that Baby B’s heart rate was dropping drastically because of the death of his twin brother. He had to be delivered immediately. Twenty minutes later both of our precious babies were delivered via emergency c-section. Kaysen Preston, our angel, weighed 3 lbs 1 oz and had passed away from getting tangled in his own umbilical cord. Our surviving twin, Tysen Lucas, weighed 2 lbs 14 oz and was taken to the NICU. I didn’t get to hear that first cry. I don’t remember much of the next 5 days. I don’t even remember meeting our sweet angel, Kaysen, for the first time. An otherwise healthy premature baby, Tysen became very sick when he was 15 days old. His premature birth resulted in him getting necrotizing enterocolitis (NEC), an intestinal illness which causes healthy bowel tissue to die. After two surgeries to remove the dead bowel, Tysen was left with only 10% of his intestines and now has what is called Short Bowel Syndrome. Short Bowel Syndrome is a condition in which nutrients are not properly absorbed because a large portion of the intestine is missing or has been surgically removed. Seven long months in the NICU and two abdominal surgeries, one heart surgery, a central line placement surgery, twenty-eight blood transfusions, and countless procedures later, Tysen came home for the first time with an ostomy, a central IV line, and a feeding tube. Although he would go on to spend another 4 months in the hospital and have several more surgeries, his health eventually stabilized. Tysen has progressed leaps and bounds since his original prognosis. We were given little hope for his survival, but Tysen has beaten the odds. He was able to have his bowels reconnected in September 2012, so he no longer has an ostomy. His bowels have been rehabilitated enough to wean him completely off IV nutrition, which means his bowels absorb all the fluids, nutrients, and vitamins his body needs to function on its own with no assistance; thus he no longer has a central IV line. He will have his feeding tube for a while to come as his bowels continue to adapt, but he does drink and eat by mouth throughout the day. Tysen is part of the Intestinal Rehabilitation Program at Children’s Mercy Hospital in Kansas City, as well as Cincinnati Children’s in Cincinnati, Ohio. These programs help “train” the remaining bowel to pick up the functions of the missing bowel, which is an ongoing, long-term process. Because Tysen is missing 90% of his bowels, staying hydrated, absorbing vitamins and nutrients, and simply growing are huge accomplishments for him. There is no cure for Short Bowel Syndrome. This is a condition he will live with for the rest of his life. Tysen has many scars to tell his story, but regardless, he always has a smile on his face. He takes things in stride and very little slows him down. He is extremely sociable and outgoing and loves showing off for people. He is the light of our lives and we can’t imagine life without him. We hold Tysen in our arms and Kaysen in our hearts. Although Kaysen is not here with us, we know that he has guided and continues to guide his twin brother, as well as his mom and dad, through all of these tribulations. 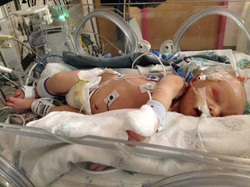 Brody was born at 39 weeks and 5 days on October 28, 2013. Even though he was born by emergency c-section, with a true knot in his cord and the cord around his neck, neither were tight and he was declared healthy. Such a miracle already!! He initially had a heart murmur and then I was told the murmur cleared. By the time he was 2 days old we were cleared to go home. At this point Brody was already beginning to eat and pee less. The next day at the pediatricians office he was again declared in good health. By Friday, at 4 days old, Brody was no longer eating and making what I thought were whimpering type noises. Being my fourth child, I didn't believe he was acting normally and my husband and I took him to the ER. We were quickly taken back, Brody taken out of arms, now completely limp. They began working on him, talking to Vanderbilt and doing what they could to keep him alive. We were told he had to be life flighted and we needed to start our drive to Nashville. We were also told there was a real chance he would not make it. We only live about 45 minutes from Vandy, but it was the longest drive ever. It is also the longest and hardest I believe I have ever prayed. We beat life flight there but once they arrived the ER doctors immediately went to work. Brody already looked better as Vandy doctors had told our ER doctors to give him prostaglandin in case it was his heart. After several touch and go moments we were told that although he was extremely sick, he was now in a more stable condition. Brody was suffering from coarctation of the aorta. When he took his first breath his PDA began closing as it was supposed to, but his aorta was also closing cutting off blood flow to the rest of his body. Brody spent 4 days in the Cardiac Care NICU. He was of course one of the largest babies, still weighing just under 8 pounds. At 8 days, the surgeon was able to go in through Brody's back and resection his aorta and reestablish proper blood flow. He had pulled through and continued to get stronger every day. Brody had another section of his aorta stop growing with his body causing another coarctation. This time, at 2 1/2 months Brody had to have his chest opened up and his aorta was patched with pericardium tissue. He is still in blood pressure medicine, has a bicuspid aortic valve and mitral valve prolapse that are both currently functioning normally. He is a true miracle, a beautiful and happy boy! I hope that the state of Tennessee - every single state- will pass a law requiring a simple pulse oximetry test before leaving the hospital. It can detect several types of heart defects. I know it would not have changed Brody's heart condition, but it would have kept him from becoming so critical. I'm so thankful to everyone that tended to him, life flight and every doctor and nurse, as well as the amount of prayers sent up on his behalf. 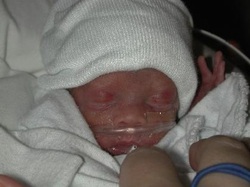 When my husband and I first found out I was pregnant, we were elated! We bought the usual books, immediately started picking out baby names and called everyone we knew. I knew that my pregnancy was going to be a breeze. Was I wrong! Six months of exhaustion, and constant morning-afternoon-night-and middle-of-the night sickness made pregnancy unbearable. When the doctor told me I had a faulty placenta and that the baby needed to be taken by emergency C-section three months early, I have to say that I was a bit relieved. ANYTHING sounded better than another three months of being pregnant! Was I wrong! And so on July 12, 2006 our son, Matt, was born. He weighed a whopping 1 pound 11 ounces and measured 12 inches at birth. He was small but mighty and during the first few weeks of his life he flourished. I just knew that our NICU stay was going to be a breeze. He was going to be home in no time! Was I wrong! After about two weeks in the NICU, things started to go downhill for Matt. He was having problems digesting his food. He was having more than his fair share of apnea episodes. His SATS were slowly lowering, eventually enough to put him back on his ventilator from which had been easily removed after only 4 days. Ultimately we found out that Matt had an infection. The doctors weren’t too concerned and so, being a new NICU mom, I wasn’t too concerned either. I knew everything was going to be fine. Give him some medicine and the “Boy Wonder” would pop right back up. No worries! Was I wrong! Matt became a very sick little boy very quickly. While he has battling his first infection, along came another one. Matt’s IV pole was filled with machines delivering all different types of medications. According to the doctors, some were for the gram negative infection and some for gram positive infection. What did that mean?? If only there was room on that pole for a little morphine! I sure could have used some to calm my nerves! Sadly, no matter what medications they pumped into Matt, nothing seemed to work. Both infections were relentless and he got sicker and sicker. Matt became septic. Sepsis occurs when chemicals released into the bloodstream to fight the infection trigger inflammation throughout the body. This inflammation can trigger a cascade of changes that can damage multiple organ systems, causing them to fail. The infections and medications were streaming through Matt’s body leaving virtually no organ untouched. Because of this, on a particularly harrowing night, his heart rate rose extremely high--to 237. It normally ranged between 170-180. His blood gases were very worrisome as well. He wasn't releasing carbon dioxide like he should and it was building up in his system. The doctors didn't know whether Matt would make it through the night. In the end, Matt surprised us all. He made it through--but not before he was put on a special respirator called an oscillator, and was pumped full of blood, platelets, and antibiotics. He was very swollen because of all of the fluids that the doctors put into him, yet he survived. The infection was still very strong, and yet he survived. It was his own strength that got Matt through that horrible night. Obviously, Matt was a very sick little boy. Sepsis was wreaking havoc on our tiny son and there were physical changes to prove it. Our tiny 1 pound 11 ounce baby was retaining so much fluid that he became a 5 pound baby overnight. He looked like Quasimodo! His skin was stretched and glassy looking. He was so swollen that the nurses were unable to close any diapers on him. His incision from a prior surgery was stretched so much that it broke open and was constantly oozing. He couldn’t open his eyes because they were swollen shut. He was a mess! The doctors were constantly telling us to hope for the best, but prepare for the worst. And just by looking at him, I knew they were right. I no longer had any delusions. The infections, the sepsis, were killing my son. Matt went on like this for a few more days. I watched while the nurses tried to make him comfortable. I watched while Matt was bounced around his bed by the huge oscillator which kept his lungs open with a constant positive end-expiratory pressure ("PEEP") and vibrated the air at a very high rate to help gases quickly diffuse in and out of the his airway. I watched while his kidneys shut down and he got more and more swollen. I watched while he slowly turned so yellow he was almost green because his liver became “insulted” by the infections. I watched while Matt had transfusion after transfusion because his platelets were non-existent. I watched as my son was slowly dying. I even signed a DNR order because the doctors told me that there was nothing else they could do and the prognosis was poor. And then, I watched as my son surprised everyone and turned a corner. For reasons unknown, Matt began to respond to the medications. He began returning negative cultures and his life got better. I can’t say that he looked any better, but his outlook looked better. And so, the doctors recommended that I rescind the DNR and that they try to fix the damage that was caused by Matt’s sepsis. The first thing they dealt with was his bloating. While Matt’s nephrologist was on his case from the beginning, he now made a life-saving decision. Since the diuretics weren’t working, he placed Matt on peritoneal dialysis to drain him of the fluid that was built up in his body. And so we spent our days in the peritoneal cycle...fill, drain, dwell. The doctor placed fluid with a special isotope into Matt’s belly. Those isotopes bound themselves to the fluid in his body. And then they drained all of the fluid from Matt. The cycle was repeated a number of times a day for two weeks and as the cycles continued, we saw Matt start to shrink. It was amazing. Matt eventually looked like the little baby he was. Once he was back to his original size, they moved on to other serious issues caused by the sepsis. Matt was diagnosed with hydrocephalus. The infections caused a blockage between the third and fourth ventricles of his brain. And so, a reservoir, and then ultimately a shunt, was placed to circulate the fluid that was building up around Matt’s brain. It was months and months before Matt returned to his normal color because his liver refused to heal itself quickly. But, eventually that was fixed as well. It is funny how a short two weeks of Matt’s life had such an impact on him and on us. Those two weeks caused Matt a lot of problems and caused his family much heartache and worry. Matt was a very sick little boy. And yet today he is running around bothering his sisters and bringing much joy to our lives. I can’t say that Matt came out of his NICU experience unscathed. And I can’t tell you we came out of it unscathed, either. But, we did make it and we are amazed and enchanted on a daily basis with our treasured son. He is a joy! Joy Tristano 7/01/14 |


 RSS Feed
RSS Feed