|
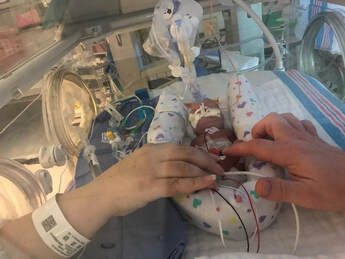
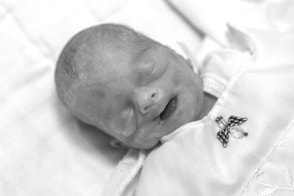
I am both a NICU mom and a loss mom. My daughter Colette died at nine days old after spending her short life in an incubator. The first time my husband and I got to hold her was as she died in our arms. Being a NICU mom is a rollercoaster for sure and my own mother, a NICU mom to my younger sister, told me just that when Colette was first born. Her advice was to just hold on and to know that starting a day off badly did not mean it ended badly and vice versa. She said it is a lot of ups and downs every day. I got a lot of similar advice from other NICU moms, nurses, doctors, and the like, but the one thing I never remember hearing was that she could die. Colette was born at 24 weeks and 5 days, after a diagnosis of severe preeclampsia and intrauterine growth restriction (IUGR) landed me in the hospital at 21 weeks pregnant. Her birth was amazing and terrifying and although we had not done a tour of our hospital’s NICU (our plan had been to do one the day she was born), I felt prepared to handle all that the NICU threw at me. Since my younger sister and I are four years apart, some of my earliest memories come from her time in the NICU and her general health and illness those first few years of her life. However much I thought I was prepared all fell away when I realized it was my daughter in that incubator and when I felt the guilt and shame that my body had failed to protect her. I had prepared myself — or at least I knew it was a possibility that she would not survive the birth. From everything the doctors had prepared us for, I knew there was the possibility that if the smallest tubes proved too big for her, then they would not be able to intervene medically, and we would hold her as she died. I even understood that the first 24 to 48 hours were touch and go. But, when she survived the birth, when the second to the smallest tube fit her, and when she made it to day three and four, I believed she would come home. I knew that her coming home would not happen quickly, and I knew that leaving the NICU was just a small step in her journey — a journey that would involve many medical issues, perhaps disabilities, lots of doctor’s appointments, and plenty of scares. While I was recovering myself from a difficult C-section, dealing with all the ups and downs of postpartum, the guilt I felt, and watching my daughter do well and then not, I was thinking of things like how we could make our house more accessible, or whether she would be able to climb stairs or not, and if we would have to makeshift or build a bedroom on the first floor. I was planning for multiple doctors’ appointments and medical equipment, never realizing that the reality would be planning for caskets and gravestones. On the day that Colette died, I still could not believe it. The doctor pulled me aside and told me what I should be prepared for and that I should call my husband and yet, I thought I knew better than all these medical professionals. Colette was not going to die, that was not in the plan, that was not what was going to happen. As the day progressed and the truth became more apparent, I still struggled to fully grasp what was happening. Even as the medical team set up our family in a private room and then walked our daughter to that room with us so we could all say goodbye, in my head, I was still in denial. There was no way that this could happen. In the four plus years that have followed since Colette’s death, I have struggled with this a lot. For as much as doctors and nurses tried to inform us of risks and dangers, I never remember being told that she could possibly die. I know I heard a lot of numbers and data about survival rates at various gestational ages, but what that really meant was never expressed to me. And for every other loss parent that I have met with a similar story of child in NICU and then their child dies, they all say something similar. I remember bonding instantly with a dad when I said that I never expected this and him saying, "oh my God me either". This experience is not as reflective of our medical system as it is of greater society. We do not like talking about death at all, but to discuss babies dying is unheard of. When we do hear about it, it is usually couched in more comfortable, digestible terms like “loss,” “survival,” etc. But the problem is that parents like us who go through these terrible tragedies are left not only to grieve, but to recover from the shock of it happening when it never appeared to be a possibility. We need to do more to help loss parents at every stage and it is well past time to start being real and direct. Tell parents that there is a risk that their child will die. Do it in a helpful, calm manner, but say it. Otherwise, we are left to struggle with even more emotions that grief brings up and as a grieving mom, the less emotions we put on the pile, the better off we are.  The views and opinions expressed in the NICU Awareness blog are those of the authors and do not necessarily reflect the official policy or position of Project Sweet Peas. About the Author Michelle Valiukenas is the proud mom of her angel Sweet Pea, who she lost due to miscarriage, her angel daughter Colette Louise who she lost at nine days old, and her only living child, her rainbow baby, Elliott Miguel. Inspired by her journey with Colette, Michelle and her husband founded The Colette Louise Tisdahl Foundation, whose mission is to improve outcomes of pregnancy, childbirth, prematurity, and infancy, as well as aid in the grieving process through financial assistance, education, and advocacy. Their flagship program financially assists families dealing with high-risk and complicated pregnancies, NICU stays, and loss. The organization’s ability to help families relies on donations and grants and they are grateful if you are able to donate. Michelle also participates and advocates on issues of maternal health, maternal mortality, infant health and safety, and pregnancy complications. Michelle lives in Glenview, Illinois with her son Elliott, husband Mark, and dog Nemo. Comments are closed.
|

 RSS Feed
RSS Feed