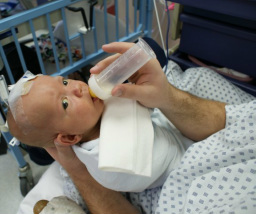
 Most parents aren’t expecting a stint in the neonatal intensive care unit (NICU) when they welcome their new baby into the world so it isn’t an experience that parents typically prepare for. Well thought out plans like how to feed your baby may have to be altered, but you do have options in the NICU. The following article is a guide to feeding in the NICU, including some of the difficult situations that parents and babies encounter depending on the baby’s level of maturity. Please reach out to your trusted health care professionals for more information and support. Overview Feeding in the NICU Babies in the NICU often have feeding difficulties because the activity requires many different body systems, which often are not fully developed. Keep in mind that you may have many steps forward and some steps back in success with feeding; do not be discouraged by this. Speech Therapy Some NICUs use speech therapists to aid with feeding therapy. At some point, the speech therapist will evaluate every infant that is admitted to the NICU to determine whether there will be feeding difficulties. According to a speech therapist, Lee Ann Damian, from Dayton Children’s Hospital “The baby’s ability to feed and gain weight is not only a survival issue, but is one of the main factors in determining how quickly that baby can go home. The sooner we can get the baby happy and comfortable with feeding, the better it will be for the entire family.” IV Therapy Upon arriving at the NICU, baby will often be too sick or even too small to bottle or breastfeed. In this case, your baby’s medical team will insert a small catheter (IV) in one of three ways -- PICC lines, peripheral IV, and Umbilical Artery Catheter. The medical team will sometimes ask you to leave the NICU unit during this insertion to better concentrate. This therapy is used to deliver fluids and medications, which baby will eventually be weaned off of. Gavage Feeding A gavage must be used for feeding of babies who are smaller or too sick to be fed by bottle or breast. A small tube will be guided through the baby’s mouth or nose into the stomach and through this tube a small amount of breast milk or formula will be trickled into baby’s stomach. Inserting this tube will cause some discomfort, but after it is in place it can be left there for up to 7 days before needing to be changed. A pacifier will often be given while gavage feeding in order to strengthen your baby’s suckling. At about 32-34 weeks of age your baby should be strong enough to start transitioning into bottle or breastfeeding. Breastfeeding in the NICU It is important to make your baby’s medical team aware of your desire to breastfeed. A collaborative effort between the mother, nurses, and lactation consultants is required for a mother to be successful with breastfeeding their NICU baby. To heighten the chance of successful breastfeeding, the baby’s mother should start pumping immediately after birth and frequently (about every 2 hours or so). The mother should make sure to pump until the breast is empty of milk, including the hind milk that is high in milk fat and essential to baby’s nutritional needs. Do not be discouraged if you are producing a small amount of milk at first. It is important to be persistent during this process. Every mother is going to produce breast milk differently. Breastfeeding in the NICU requires an enormous amount of patience. Preemies and sick babies take a long amount of time to learn the coordination of suckling, breathing, and swallowing. A popular method to start the breastfeeding process is Kangaroo Care, a method that involves skin-to-skin contact. During this process, the baby, clothed only in a diaper, will be snuggled up to your bare chest. This can be done by either the mother or father for several hours a day. Kangaroo Care has many benefits, including heart rate stabilization, increased weight gain, and will lead to a better chance to breastfeed. Parents feel some additional benefits from Kangaroo Care, such as increased sense of control, increased milk production, bonding, etc. Another helpful method is to introduce a pacifier dipped in breast milk. This helps promote suckling. Kangaroo Care creates more opportunity for baby to “go to the breast.” This is a time for the baby to explore and smell mother’s nipple. It is important to pump before going on to this step so there will not be too much milk. Remember it takes the coordination of suckling, breathing, and swallowing on your baby’s part to be successful so it is central to be very patient. Formula Feeding in the NICU Although formula feeding might not have been your first option, your baby can thrive with this method too. There are many formula options and your NICU team will assist with picking the one best suited for your baby’s needs. Although your baby’s time in the NICU will most likely include some challenges with feeding, there are many methods (many not included within this article) and skilled professionals to help you and your baby overcome them. Resources Feeding Matters mission is to bring pediatric feeding struggles to the forefront so infants and children are identified early, families' voices are heard, and medical professionals are equipped to deliver collaborative care. Feeding Matters overcome the complex issues of pediatric feeding struggles through our five mission pillars: Education, Advocacy, Research, Treatment, and Support. Oley Foundation enriches the lives of those requiring home intravenous and tube feeding through education, outreach, and networking.Feeding Matters brings pediatric feeding struggles to the forefront so infants and children are identified early, families' voices are heard, and medical professionals are equipped to deliver collaborative care. La Leche League supports mothers worldwide to breastfeed through mother-to-mother support, encouragement, information, and education Feeding Tube Awareness Foundation dedicated to providing parents and caregivers with the information needed for day-to-day life with a child who is tube-fed. Women, Infants and Children (WIC) provides Federal grants to States for supplemental foods, health care referrals, and nutrition education for low-income pregnant, breastfeeding, and non-breastfeeding postpartum women, and to infants and children up to age five who are found to be at nutritional risk. GI Kids provides easy to understand information about the treatment and management of these pediatric digestive conditions for children and parents Hand to Hold provides comprehensive navigation resources and support programs to parents of preemies, babies born with special health care needs and those who have experienced a loss due to these or other complications. United States Breastfeeding Committe (USBC): The mission of USBC is to improve the Nation's health by working collaboratively to protect, promote, and support breastfeeding. WIC The Special Supplemental Nutrition Program for Women, Infants, and Children (WIC) provides Federal grants to States for supplemental foods, health care referrals, and nutrition education for low-income pregnant, breastfeeding, and non-breastfeeding postpartum women, and to infants and children up to age five who are found to be at nutritional risk. PLEASE NOTE: The contents of this article is for informational purposes only. Nothing contained in this article should be considered or used as a substitute for professional medical or mental health advice, diagnosis, or treatment. References "How to Feed your NICU Baby." Bay State Health. N.p., n.d. Web. 14 Sept. 2014. <http://baystatehealth.com/Baystate/Main+ "In the NICU." Feeding your baby in the NICU. N.p., 1 Aug. 2014. Web. 14 Sept. 2014. <http://www.marchofdimes.org/baby/feeding-your-baby-in-the-nicu.aspx>. "Meeting the Challenges of Breast-Feeding in the NICU." Pregnancy.org. N.p., n.d. Web. 14 Sept. 2014. <http://www.pregnancy.org/article/meeting-challenges-breast-feeding-nicu>. "NICU Feeding Baby Steps." The Chester County Hospital. N.p., n.d. Web. 14 Sept. 2014. <http://www.chestercountyhospital.org/cchpage.asp?p=1424>. "Pediatric Dysphagia." : Overview. Web. 14 Sept. 2014. http://www.asha.org/PRPSpecificTopic.aspx?folderid=8589934965§ion=Assessment. "Speech therapy in the NICU: Key to babies' survival." Speech therapy for premature newborns : The Children's Medical Center of Dayton. Web. 14 Sept. 2014. http://www.childrensdayton.org Comments are closed.
|
 RSS Feed
RSS Feed