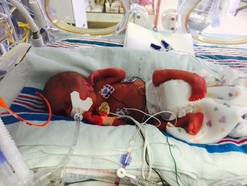
 When Kelly Guzman discovered she was pregnant she was overjoyed, and since it was her first, she was blissfully unaware that anything could go wrong. According to her, it was a difficult pregnancy; she lost weight and barely had an appetite. But she continued to visit her physician who assured her everything was going smoothly. At her 20 week exam she discovered they were expecting a boy, who her and her partner named Joshua. The doctors also thought they noticed some abnormalities, and became insistent that the baby had a genetic deformity. If she didn’t miscarry, the doctors strongly recommended aborting the baby. To this, Kelly firmly resisted. At 27 weeks, Kelly started experiencing sharp pains and debilitating nausea. As it turns out, she was suffering through the early symptoms of HELLP syndrome, and could have bled out or potentially lost the baby at any moment. A week later she underwent an emergency C- section which required 3 blood transfusions to bring her platelet count up to a survival level. Joshua was still-born, but miraculously revived, weighing just 1 pound, 11 ounces and severely jaundiced from oxygen deprivation. Joshua was so small because he was restricted to growing only on the left side of Kelly’s uterus, as she also had an undiagnosed uterine abnormality, a bicornuate uterus. Because this was her first baby, there was no way she could have ever known she had this irregularity. After being in the St. Mary’s NICU in West Palm Beach, FL for 7 seven days, Joshua was transferred to Nicklaus Children’s Hospital in Miami, as he had suffered a grade 3 brain bleed with enlarged ventricles. Joshua’s limited oxygen also lead to an excessive amount of folding on the brain, called polymicrogyria, which can cause seizures. For the ensuing 140 days, Kelly and her partner drove the 2-3 hour drive every weekend to watch over Joshua and comfort him as best they could. Finally, at 8 weeks old and on her birthday, Kelly was able to hold her son. They weren’t clear of all troubles yet, as Joshua still needed surgery to close a flap near his heart which had not fully healed. He had also developed chronic lung disease and bronchopulmonary dysplasia, because he was required to be on ventilator support throughout his stay in the NICU. Not being able to see Joshua daily, coupled with the fact he was kept sedated, were the hardest parts for the parents. In order to keep him calm and to help accept the life support, Joshua was on a constant drip of either morphine or fentanyl for his entire stay. The withdrawal effects of these drugs were especially painful, and the reason he needed to stay so long in the Nicklaus NICU. After 147 days in two NICUs, Joshua was finally released, weighing just over 6 pounds. Kelly is happy to report that a year after his discharge, Joshua is doing perfectly fine, with no genetic abnormalities or residual complications. He is crawling, taking his first steps and saying his first words. After going through a pregnancy complicated by HELLP syndrome and an extensive stay in a NICU, Kelly hopes that her story can be an example of not only what can go drastically wrong, but what can go unexpectedly right. Pregnancy Complications – Preeclampsia and HELLP Syndrome A variety of complications can arise unexpectedly during pregnancy, causing many women to have a very difficult experience. This sometimes can be due to the personal health factors of mother, which when left unnoticed, lead to problems as the pregnancy progresses. The severity and type of challenges can truly run the gauntlet for women, from the onset of gestational diabetes, to premature labor and miscarriage, to severe and persistent nausea and vomiting (hyperemesis gravidarum).[i] One of the most critical and life-threatening problems that can occur is preeclampsia, and its severe variant HELLP syndrome, which are characterized by the sudden onset of high blood pressure and protein in the urine. Historically, preeclampsia has always affected a certain portion of pregnant women. From the time of Hippocrates up until the 20th century, physicians were not only baffled by how these symptoms developed, but in how to treat them successfully. The most common methods were bloodletting, elimination of toxins, rest and purging. These treatments were prescribed for millennia, and did not change all that much until doctors started to understand the pathophysiological changes that are the symptoms of this condition; notably the increase in blood pressure and presence of protein in the urine. Due to their research from the second half of the 20th century up until today, physicians have learned how to better treat the symptoms, but still cannot prevent the disorder’s occurrence.[ii] Unfortunately it is still mostly unknown how and why preeclampsia develops in pregnant women, however, doctors believe it is related to the poor development of blood vessels in the placenta. This condition affects between 5-8% of all pregnancies in the United States, and only through proper prenatal care and by watching for warning signs can it be caught early and managed.[iii] A more acute form of preeclampsia is HELLP syndrome, (hemolysis, elevated liver enzymes, low platelet count). The symptoms of HELLP are similar to that of preeclampsia, high blood pressure and protein in the urine, but can also involve chest pain, pain when breathing, edema and uncomfortable indigestion. This particular disorder is very hard to diagnose, as its symptoms can sometimes be mistaken for the flu. If is not caught in time, it can lead to liver rupture or stroke, and put the life of the mother and child at risk. Of the 5-8% of U.S. women who will develop preeclampsia, roughly 15% of those women will develop indications of HELLP syndrome.[iv] Since it is still unknown how these symptoms arise, it is important for physicians to consistently run blood tests and urine samples for any woman experiencing any signs of HELLP during her third trimester. Treatment options for HELLP are weighed against the gestation of the pregnancy, as the best solution for mom and baby is a delivery. Since physicians do not know precisely how and why these symptoms progess during pregnancy, there can be no way to completely prevent it. They recommend monitoring diet and exercise, and regular prenatal visits to observe blood pressure.[v] By ensuring that women are informed and aware of any changes however slight to their blood pressure, they can seek help when severe warning signs develop such as violent pains and severe nausea. By staying attentive to their bodies, women who may be experiencing the first signs of preeclampsia or HELLP will greatly increase their chances of survival and safe delivery of their baby. [1] https://www.nichd.nih.gov/health/topics/pregnancy/conditioninfo/pages/complications.aspx
[1] http://www.preeclampsia.org/history-of-preeclampsia [1] http://www.mayoclinic.org/diseases-conditions/preeclampsia/basics/definition/con-2003164 [1] http://www.preeclampsia.org/health-information/53-health-information/57-hellp-syndrome v http://americanpregnancy.org/pregnancy-complications/hellp-syndrome/
Lisa Ritenour
9/3/2016 05:35:09 pm
God Bless him! He is a gorgeous baby! My son was also in the NICU at Nicklaus Children's Hospital. They are the absolute best! They take such good care of our babies! So happy to hear your son is doing so well! Enjoy every moment!
Jenice Grzeszczak
9/3/2016 09:36:30 pm
I also had HELLP Syndrome and had to give birth via emergency C-Section at 27 weeks. I am so happy that you and your little one made it safely through that scary time!
Lauren Weber
5/17/2018 04:53:40 pm
I also had HELLP and delivered at 27 weeks to find out I have a uterine abnormality. I am SO touched by Joshua's story. My little boy is 9 months old now and also doing well. It really helps me to hear other's stories. Comments are closed.
|



 RSS Feed
RSS Feed